I knew something was wrong but I didn’t want to go to the doctor.
And that was the situation for many during COVID quarantines. Where I live, emergency room visits dropped by more than half in the month after shutdown, and a month later they had only risen to 60% of normal. Knowing that only about 20% of emergency visits are unnecessary, public health officials urged residents to not be afraid of infection and go if they needed to.
Still, I debated long and hard before I woke my son up early one morning and asked him to drive me in. It was the thought of him being the one to find me if I died in my bed that finally pushed me to it.
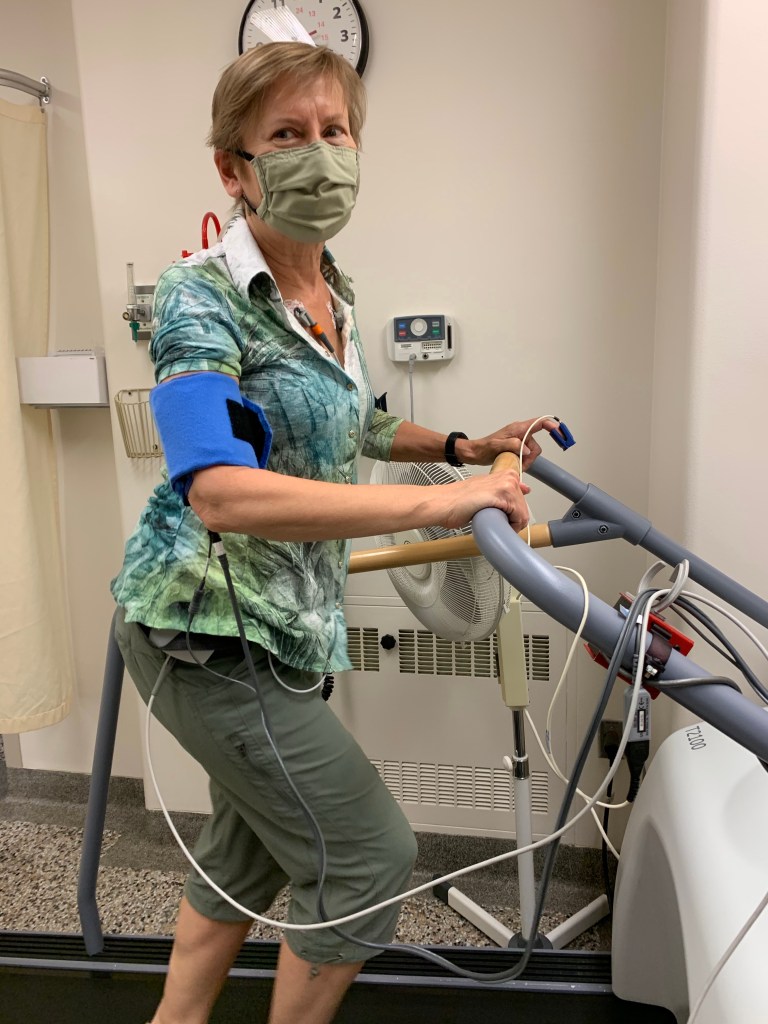
I’m fine now, by the way. However in the quest to discover why someone who could hike the grueling Incan Trail would, 4 months later, be unable to make it up a single flight of stairs without stopping and gasping, I had an inside look at the medical system in the time of Covid.
First, there are no crowds. The majority of my doctor’s appointments were by phone. When visiting in person, I would wait in my car and the staff member who texted me to come in would unlock the door and take me directly to an examination room. At hospitals, preliminary screening takes place outside or at the door, unless you arrive by ambulance. If I hadn’t had my own mask, I would have been given one to go with the ubiquitous shot of hand sanitizer.

If you need to wait, outside a testing room or lab, every second chair is taped off for distancing. Most staff are wearing masks. Several doctors were not, but that was after I had a negative Covid test. After the first phone consultation with my doctor she sent me to a respiratory centre, a trailer in the back parking lot of the hospital, where a physician in full PPE took the swab as part of my examination.

Increased cleaning means everything takes longer, but health care workers are adjusting and adapting. In emergency I overheard a briefing on standardizing tubing sizes between departments to reduce the need to change them. Over three months of visiting labs and hospitals, I have seen these health professionals deal quietly with what is just, to them, enhanced protocols.
Like all of us, they have gone through stress and worry. Although they likely appreciated the healthcare worker salute we gave every day at 7 pm, I’m sure many of them wondered how they ended up literally putting their lives on the line. That was not what they signed up for. Yet they continue to do their jobs, calmly and professionally.
We avoided the first surge that overwhelmed hospitals in many parts of the world. Despite early outbreaks, British Columbia controlled the spread and has had less than 5000 cases and just over 200 deaths. But cases are climbing again, more than in those initial months.
Our healthcare workers are prepared. I hope we can do our part to make those preparations unnecessary.